How OCT Works
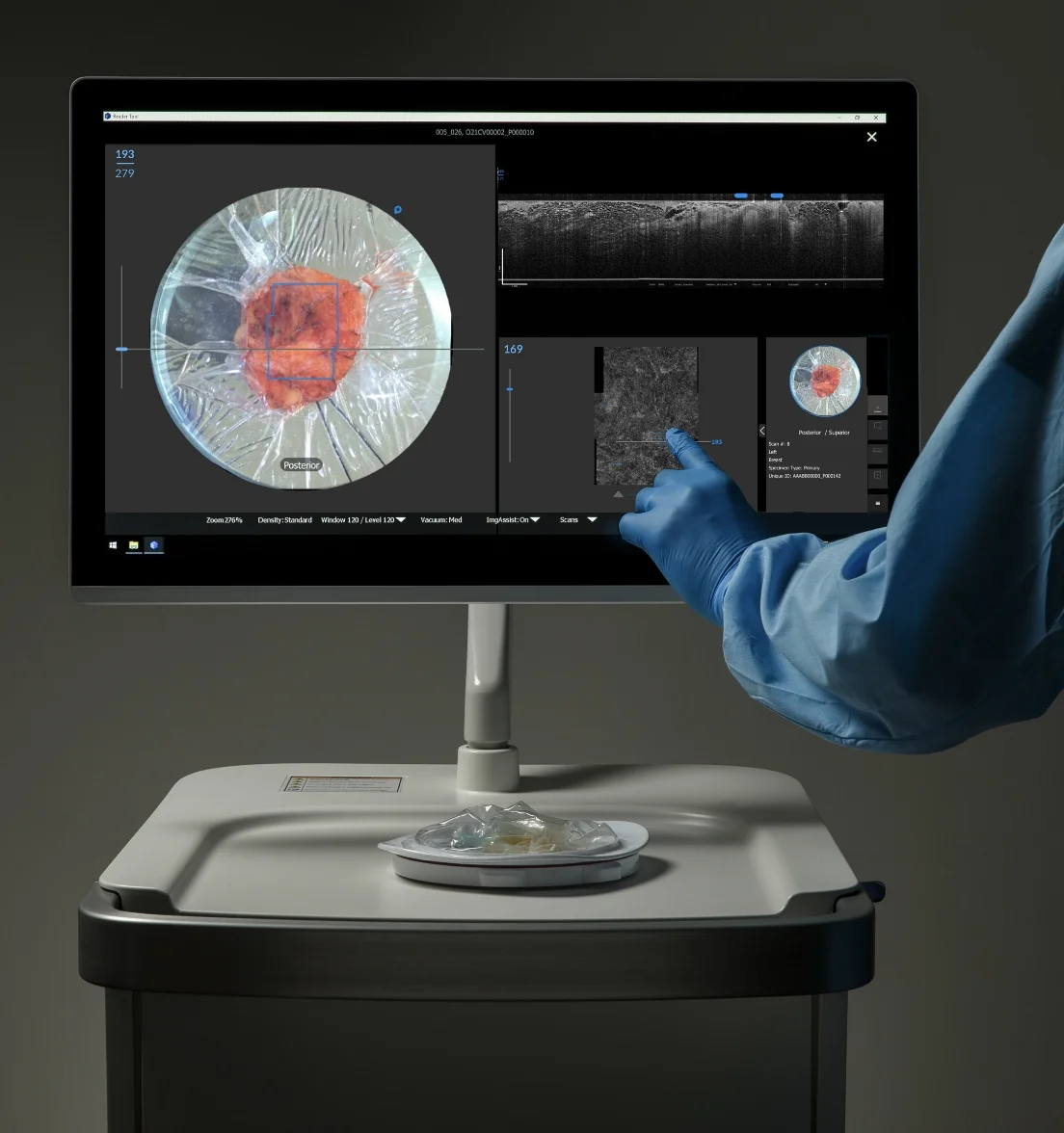
Think of Optical Coherence Tomography (OCT) as an “ultrasound with light.” It works similarly to a traditional ultrasound, but it uses light instead of sound to create a high-definition 3D scan of microscopic details with much higher resolution.